The Industry’s Highest Standards for Vendor Compliance
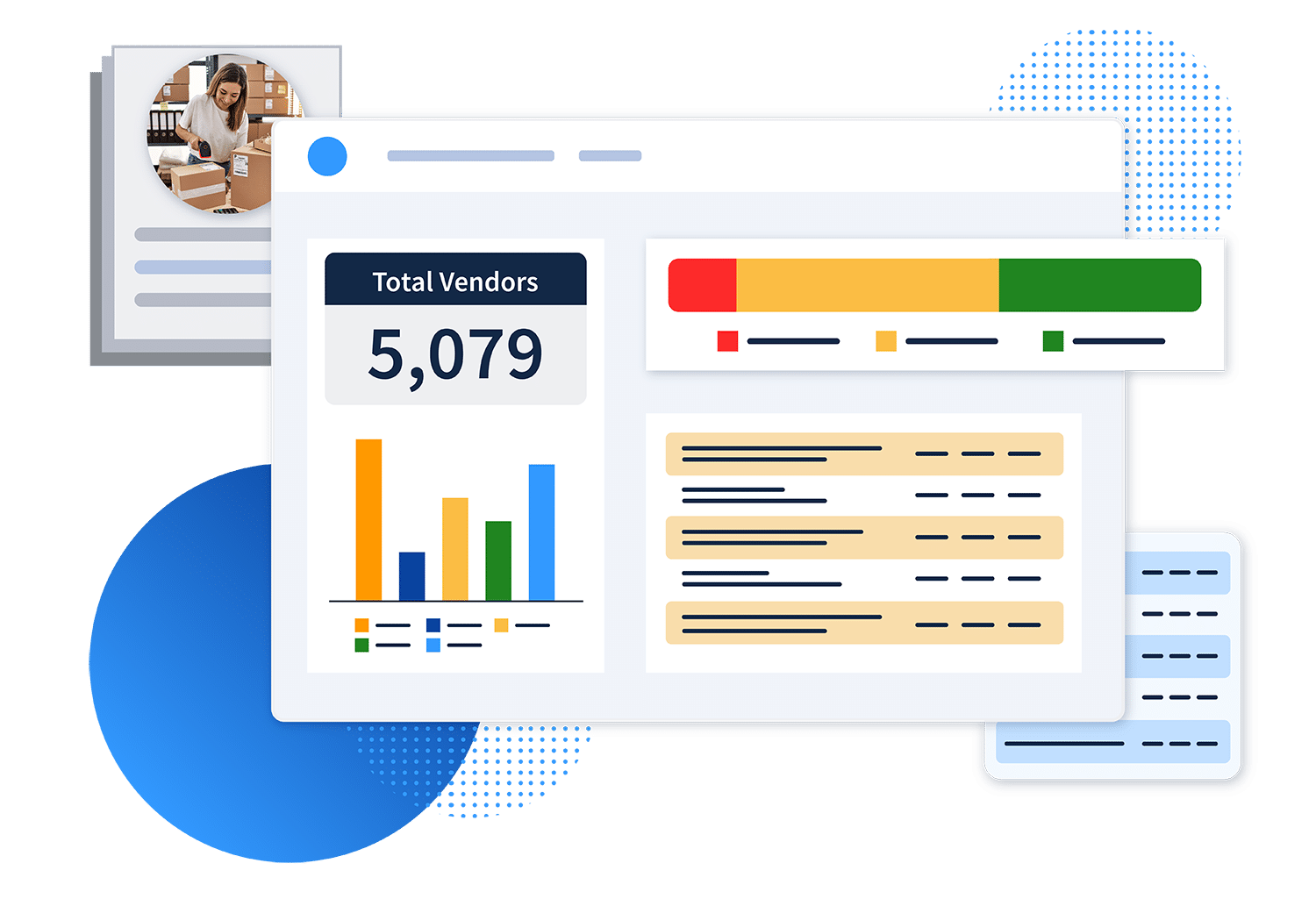
360-Degree Vendor Compliance Oversight
Setting a New Gold Standard for Vendor Compliance
Vendors make up a crucial segment of the healthcare ecosystem, and yet vendor compliance remains a black hole for many healthcare organizations. Our comprehensive vendor compliance solution shines a light on this hard-to-monitor population, continuously checking federal and state exclusion lists for vendor entities, owners, or employees that your organization engages.
Our strategic approach includes annual vendor data collection and ongoing vendor owner and employee monitoring, plus verification of data integrity and continued maintenance to prevent stale data. We offer bi-directional financial benefits including resource support for implementation, so this step toward eradicating fraud, waste, and abuse can also help protect your bottom line.
What We Deliver:
- Vendor outreach on the client organization’s behalf
- Vendor onboarding and approval workflows to ensure vendor eligibility
- Annual collection and consolidation of disparate vendor data
- Identification of vendor entity and ownership
- Complimentary, ongoing federal & state exclusion monitoring for vendor populations
Annual Vendor Data Collection
Let us handle the vendor outreach
Guaranteed vendor participation

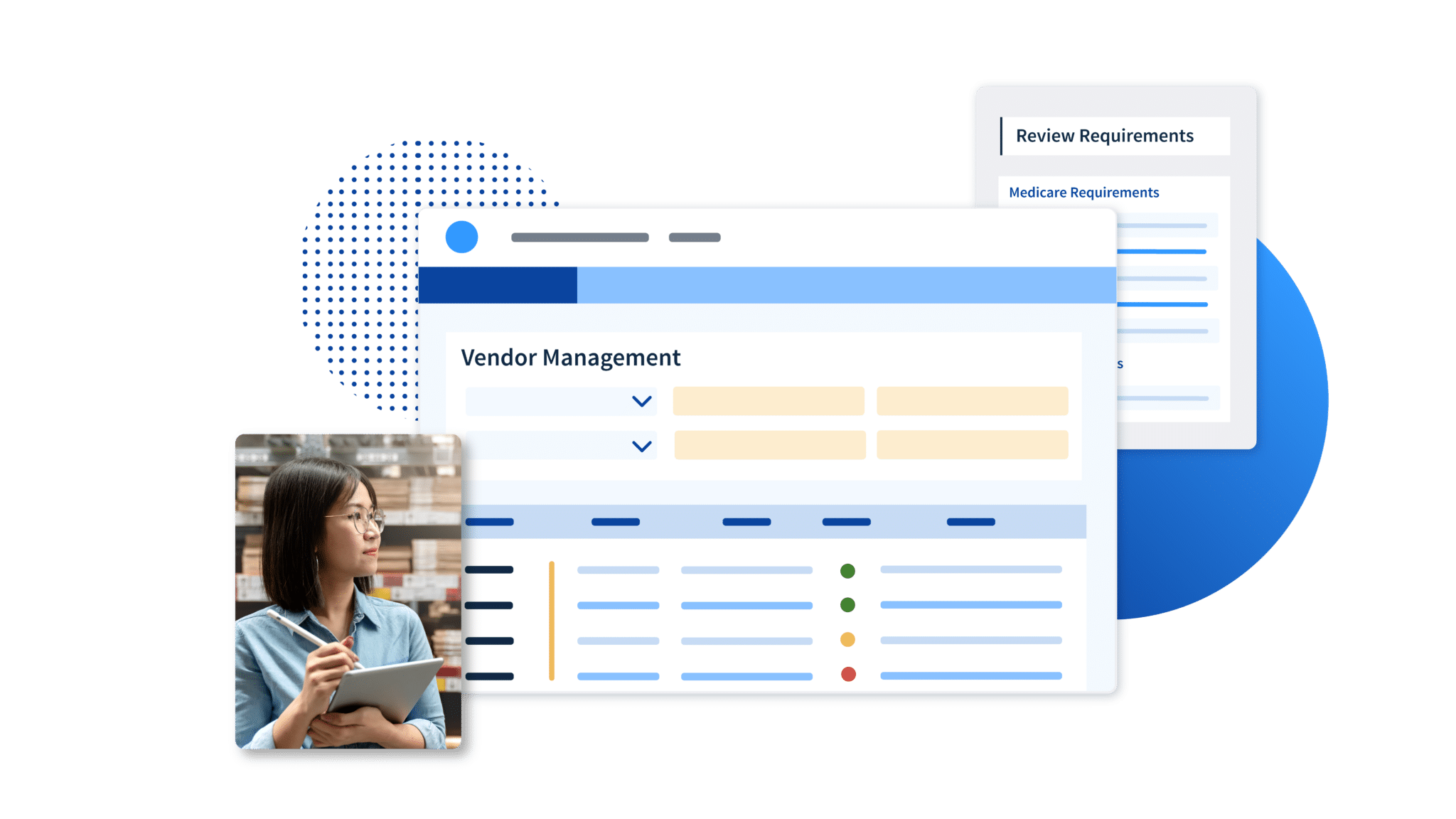
Ongoing Vendor Owner and Employee Monitoring
Uphold data integrity
Comprehensive coverage for your full vendor population
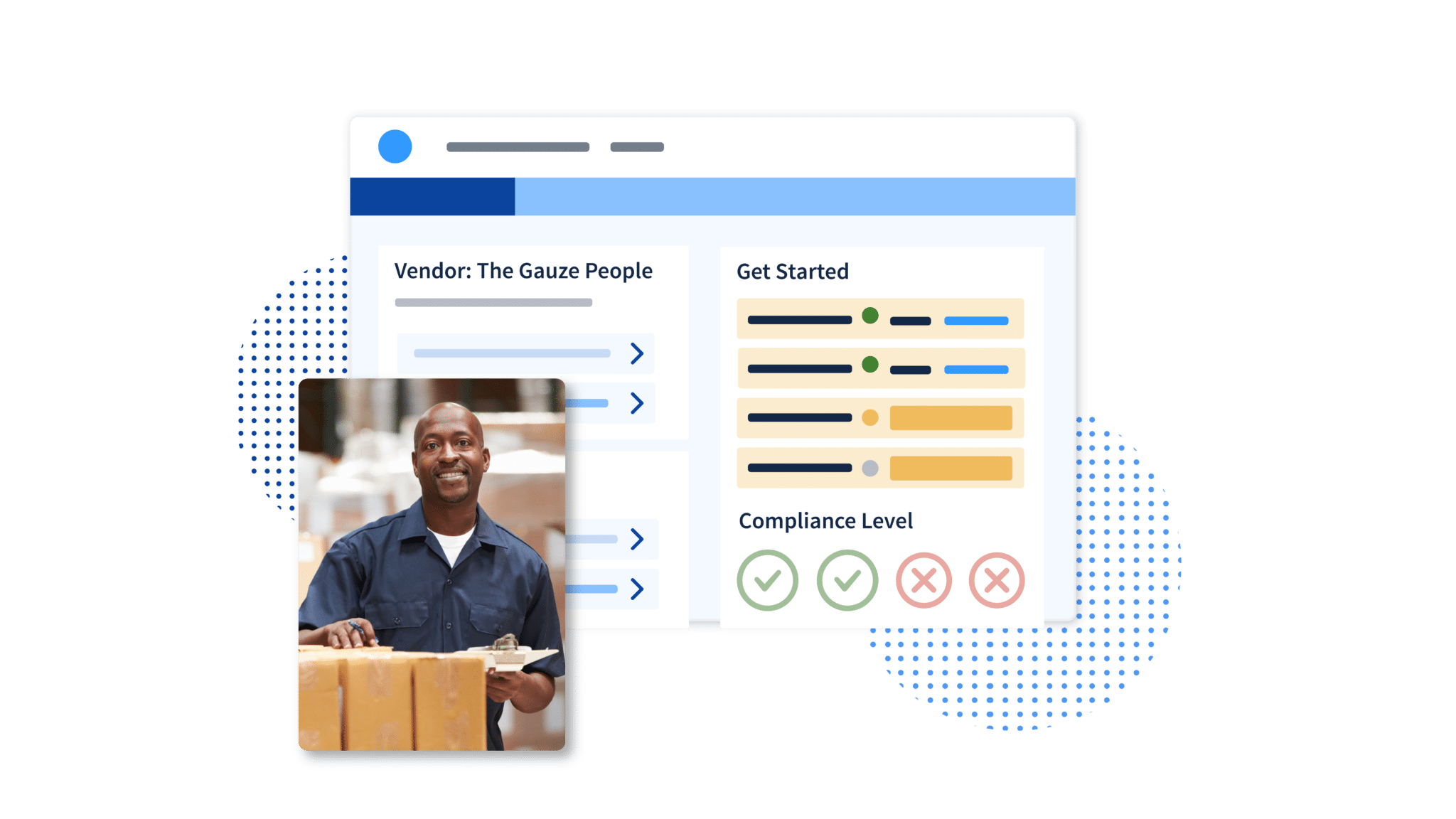
Ensure Better Supply Chain Management
Only contract with eligible vendors
Directly integrate with your current AP system
For Compliance Leaders
Impact Compliance™
Together, we can impact change.
Introducing the industry’s highest standards in healthcare compliance monitoring. This comprehensive program provides organizations across the care continuum with a roadmap to implement above-average compliance practices by:
- Addressing key population monitoring gaps
- Prioritizing financial efficiencies
- Upholding community healthcare and success




“Not only has ProviderTrust saved us countless hours of unnecessary work and delivered peace of mind that no exclusions will be missed, but their solution is also the most polished one that we work with and we are frequently complimented on how organized our credentialing files and programs are.”

“Most healthcare companies know how to check the OIG website, but checking all the state Medicaid sites, SSDMF, and all other sources is where ProviderTrust really provides us a great service.”
Integrate Your Applications with ProviderTrust




















