The latest HHS OIG release of the Semiannual Report to Congress comes at a time when the agency has been facing turnover in leadership while balancing being able to provide transparency and data around many of the challenges involving COVID-19. For this post, we’ll take a look at some of the highlights from the report and areas of interest for federal healthcare programs moving forward.
Leadership Turnover in HHS OIG
Have you noticed the different names associated with the latest HHS OIG reports? The HHS Office of Inspector General has experienced multiple leadership turnover challenges, as the latest acting Principal Deputy Inspector General, Christi A. Grimm, has been replaced by President Trump. Prior to Grimm, her predecessor Joanne M. Chiedi resigned in December 2019.
Both former HHS OIG leaders had short-lived stints after Daniel Levinson resigned after 15 years as Inspector General. The level of turnover raises some concern about the current operations for the agency, as well as uncertainty about the future as the Trump administration has nominated Jason Weida, an assistant United States attorney in Boston, as permanent Inspector General. His assignment will still need to be approved by the Senate before he is able to serve as the next HHS OIG Inspector General.
A Message from Christi A. Grimm
Christi A. Grimm, Principal Deputy Inspector General presented the Spring HHS OIG Semiannual Report to Congress. In her summary, she described some of the latest efforts to protect federal healthcare programs and described some examples of fraud, waste, and abuse. Notable mentions from the report included an audit that found poor interagency communication and internal management decisions failed to protect children’s interests and left HHS unprepared for the zero-tolerance policy.
HHS OIG Semiannual Report to Congress
What is the HHS OIG Semiannual Report to Congress?
The OIG Semiannual Report to Congress describes OIG’s work on identifying significant problems, abuses, deficiencies, remedies, and investigative outcomes relating to the administration of HHS programs and operations that were disclosed during the reporting period. In the report, OIG publishes expected recoveries, criminal and civil actions, and other statistics as a result of their work for the semiannual reporting period.
The HHS Office of Inspector General (OIG) has released its latest version of the 2020 Spring Semiannual Report to Congress to summarize OIG activities from October 1, 2019 – March 31, 2020. To reference previous archived reports, check here – OIG Semiannual Reports Archive. Below, you will find some of the highlights, focus areas, results, and more from HHS OIG during the reporting period.
HHS OIG Work Plan
Each month, OIG releases their Work Plan updates to inform the public about the projects they are taking on during the year including auditing, reporting, and investigating HHS operating divisions, including the following:
- Centers for Medicare & Medicaid Services (CMS)
- Public health agencies such as the Centers for Disease Control and Prevention (CDC)
- National Institutes of Health (NIH)
- Administration for Children and Families (ACF)
- Administration for Community Living (ACL)
- Various state and local governments – evaluating the use of federal funds as well as the administration of HHS.
*Some of the projects described in the Work Plan are statutorily required.
HHS OIG 2020 Accomplishments and Excluded Individuals and Entities
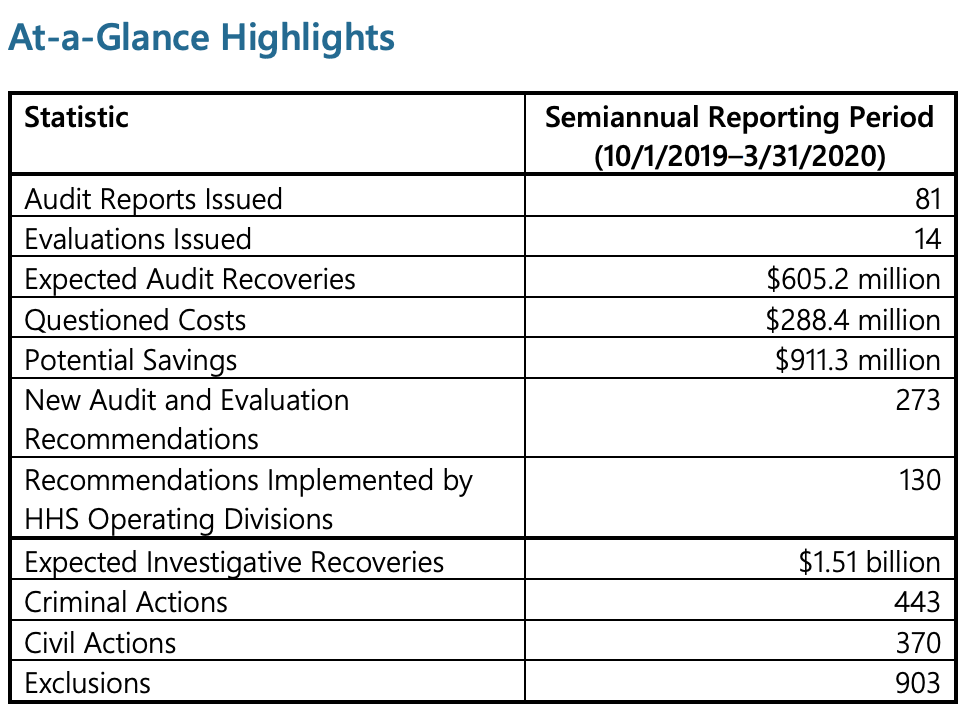
OIG’s investigative work led to $1.51 billion in expected investigative recoveries and 443 criminal actions during this reporting period. OIG also took civil actions, such as assessing monetary penalties, against 370 individuals and entities, and excluded 903 individuals and entities from federal health care programs. OIG audit work also identified $911.3 million in potential savings for HHS— funds that could be saved if HHS implemented all of OIG’s audit recommendations.
Preparing for and Responding to the COVID-19 Pandemic and Other Public Health Emergencies
In March, HHS OIG released a COVID-19 Portal to help provide details for oversight and enforcement actions, as well as general questions during the personal health emergency. The portal also helps provide valuable information regarding COVID-19 fraud, infectious disease preparedness and response protocol, and government policy statements and guidance.
HHS ASR has utilized the Technical Resources, Assistance Center, and Information Exchange (TRACIE) to host information for healthcare organizations to find the latest centralized Novel Coronavirus Resources. The gateway helps provide the latest information on new important initiatives and guidance for emergency preparedness, telehealth delivery, securing personal protective equipment (PPE), and much more.
View our On-Demand webinar to learn more about how Compliance and Human Resource professionals are working together to respond to COVID-19.

Fighting Fraud To Protect the Medicare and Medicaid Programs
Key Medicare Tools To Safeguard Against Pharmacy Fraud and Inappropriate Billing Do Not Apply to Part D (OEI-02-15-00440), March 2020
Page 21
Medicare Part D does not have three key tools to protect against pharmacy fraud that are available in other parts of Medicare: pharmacy enrollment, revocation, and preclusion. These three tools apply to pharmacies only when they bill Parts B or C, not when they bill Part D. We continue to recommend that CMS require pharmacies that bill Part D to enroll in the Medicare program. This was an integral part of a previous recommendation that CMS has yet to implement. CMS concurred with all three of our new recommendations, which were:
- Allow revocation of Medicare enrollment for inappropriate billing of Part D
- Include on the Preclusion List pharmacies that inappropriately bill Part D
- Apply the Preclusion List payment prohibitions to pharmacies and other providers that dispense Part D drugs
Ohio—Ryan P. Sheridan, owner and operator of Braking Point Recovery Center
Page 37
Ryan P. Sheridan, owner and operator of Braking Point Recovery Center, was convicted of charges from his involvement in a $48 million scheme to defraud Medicaid. Sheridan also owned and operated numerous other businesses, including Braking Point Health and Fitness LLC and Braking Point Recovery Housing LLC, which owned recovery houses (or “sober houses”) for individuals attempting to maintain abstinence from drugs and alcohol.
According to court documents, between January 12, 2015 and October 18, 2017, Sheridan and his codefendants submitted or caused to be submitted billings to Medicaid for drug and alcohol services that were: coded to reflect a service more costly than was actually provided; without proper documentation; without proper assessment documents containing valid diagnosis; billings for patients whose records did not contain diagnosis by a physician; related to treatment at unlicensed inpatient beds; billings related to dispensing of Suboxone, even though the treating physician did not have the authority to do so; for Department of Health and Human Services, Office of Inspector General Semiannual Report to Congress—October 1, 2019, through March 31, 2020 38 case management services when, in fact, the clients were working out at Sheridan’s gym; billings based on quotas provided to the nurses by the defendants to bill 4 to 5 hours of treatment daily, even if the services were not medically necessary; billing for inpatient detox and drug treatment services that were, in fact, provided in an outpatient setting, among other violations.
Are you protecting your healthcare organization from fraudulent vendors, owners, and managers?
[button text=”Get the details on vendor onboarding ” link=”solutions/vendor-onboarding/” class=”button-blue-text” arrow=”true”]
Home Health Agency Fraud Continues to Increase
Page 39
Florida—Rodolfo and Marta Pichardo were sentenced to prison for their roles in a $38 million health care fraud and wire fraud scheme. According to court documents, the Pichardos built a vast empire of fraud, consisting of at least six fraudulent home health agencies, three fraudulent therapy staffing companies, and two fraudulent pharmacies. Each of these entities purportedly provided home health services, therapy services, and prescription drugs, respectively, to qualified Medicare beneficiaries, though in fact they did not.
From May 2010 through September 2016, the Pichardos and their co-conspirators used this empire to submit more than $38 million in fraudulent claims to Medicare, for which the trust-based program then paid out more than $33 million. The Pichardos then used this money to purchase multiple properties, high-end vehicles, expensive jewelry, plane tickets, vacations, cosmetic procedures, and more, both for themselves and their family members. As part of the scheme, Rodolfo Pichardo offered and paid kickbacks, both by cash and by check, to numerous patient recruiters, in exchange for the referral of Medicare beneficiaries to home health agencies that he owned.
The conspirators also offered and paid cash kickbacks to owners and operators of multiple Miami-Dade medical clinics, in return for acquiring medically unnecessary home health prescriptions for the recruited Medicare beneficiaries. These prescriptions were then used by the Pichardos’ various home health agencies and pharmacies to bill Medicare for purported services and pharmaceutical drugs that were provided to allegedly qualified Medicare beneficiaries.
Rodolfo and Marta were sentenced to a total of 23 years and 8 months in prison and ordered to pay $33.8 million in restitution, joint and several with a codefendant. Four defendants involved in the scheme were previously sentenced to a combined 12 years and 1 month in prison and ordered to pay $135,245 in restitution.
Learn more about the increases in home health agency fraud
[button text=”More articles this way ” link=”blog/vulnerabilities-personal-care-home-health-services/” class=”button-blue-text” arrow=”true”]
HHS OIG Top 3 Goals for Protecting the Integrity of Federal Healthcare Programs
Christi A. Grimm concluded by mentioning HHS OIG top three goals: to fight fraud, waste, and abuse; to promote quality, safety, and value in HHS programs and for HHS beneficiaries; and to advance excellence and innovation.
We do this through data-driven reviews and investigations, supported with modern auditing, investigative, and evaluative methods, and a team of over 1,600 dedicated public servants. Impact. Innovation. People focus. These are the core values that inspire OIG to serve the American public with independent, objective oversight.”
– Christi A. Grimm, Former Principal Deputy Inspector General
ProviderTrust Aims to Make Healthcare Smarter and Safer
A recent Johns Hopkins Bloomberg School of Public Health study described how patients of Medicare providers committing fraud and abuse are more likely to be disabled or have low income. Our team is dedicated to assisting healthcare organizations to keep patients safe and improve the value of care with our automated solutions.
We work with a wide variety of customers from small independent health centers to large national health plans to ensure federally funded compliance standards are met, and that the best healthcare is being delivered safely.
The ProviderTrust difference is in our data. We deliver the best quality healthcare data with advanced sorting algorithms to filter out the most important information from government databases, registries, accreditations, licensing boards, and more.
We then augment your data with unique identifiers to find exact-matches, saving you time and mitigating the risk of fraud, waste, and abuse (FWA). To learn more, feel free to Contact Us at any time.
Interested in learning more?
[button text=”More HHS OIG Resources This Way” link=”tag/oig/” class=”button-blue-text” arrow=”true”]









