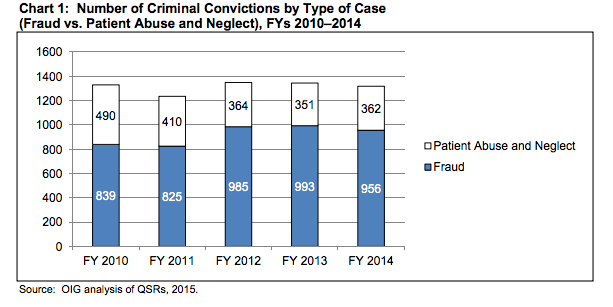
According to the OIG Report on 2014 Medicaid Fraud Control Unit performance, about three quarters of the criminal convictions from the MFCU involved healthcare fraud and abuse. A quarter of that fraud involved patient abuse and neglect. Convictions related to fraud consistently represented the majority of all criminal convictions over the past five years.
A breakdown of the types of criminal convictions, per category demonstrate convictions for:
1. Fraud
- Conspiracy to commit healthcare fraud and abuse.
- Submitting false statements related to healthcare matters.
- Making false statements in regard to healthcare reimbursements.
- Grand larceny.
- Violations of anti-kickback statutes.
- Improperly prescribing drugs.
2. Abuse and Neglect
- Aggravated assaults.
- Injury to Elderly or Disabled persons.
- Theft of Patient Funds.
Summary:
MFCU’s play an important and necessary role in feretting out and deterring, as well as prosecuting, healthcare fraud and abuse. Civil fines imposed and criminal convictions are vital to the role of MFCU’s in the aim to stop and punish those for fraud and abuse in healthcare compliance industry.
You might also enjoy:
OIG Exclusion vs. Termination
MFCU performance not measuring up
North to south – MFCU not reporting all OIG exclusions
How well are the medicaid fraud control units doing?

Written by Michael Rosen, ESQ
ProviderTrust Co-Founder, mrosen@providertrust.com
Michael brings over 20 years of experience founding and leading risk mitigation businesses, receiving numerous accolades such as: Inc Magazine’s Inc 500 Award and Nashville Chamber of Commerce Small Business of the Year
Connect with Michael on Linkedin