Fast, Accurate Provider Credentialing for Payers
Speed up turnaround times by 97% and ensure the accuracy of your results with ProviderTrust’s HITRUST- and NCQA-certified primary source verifications.
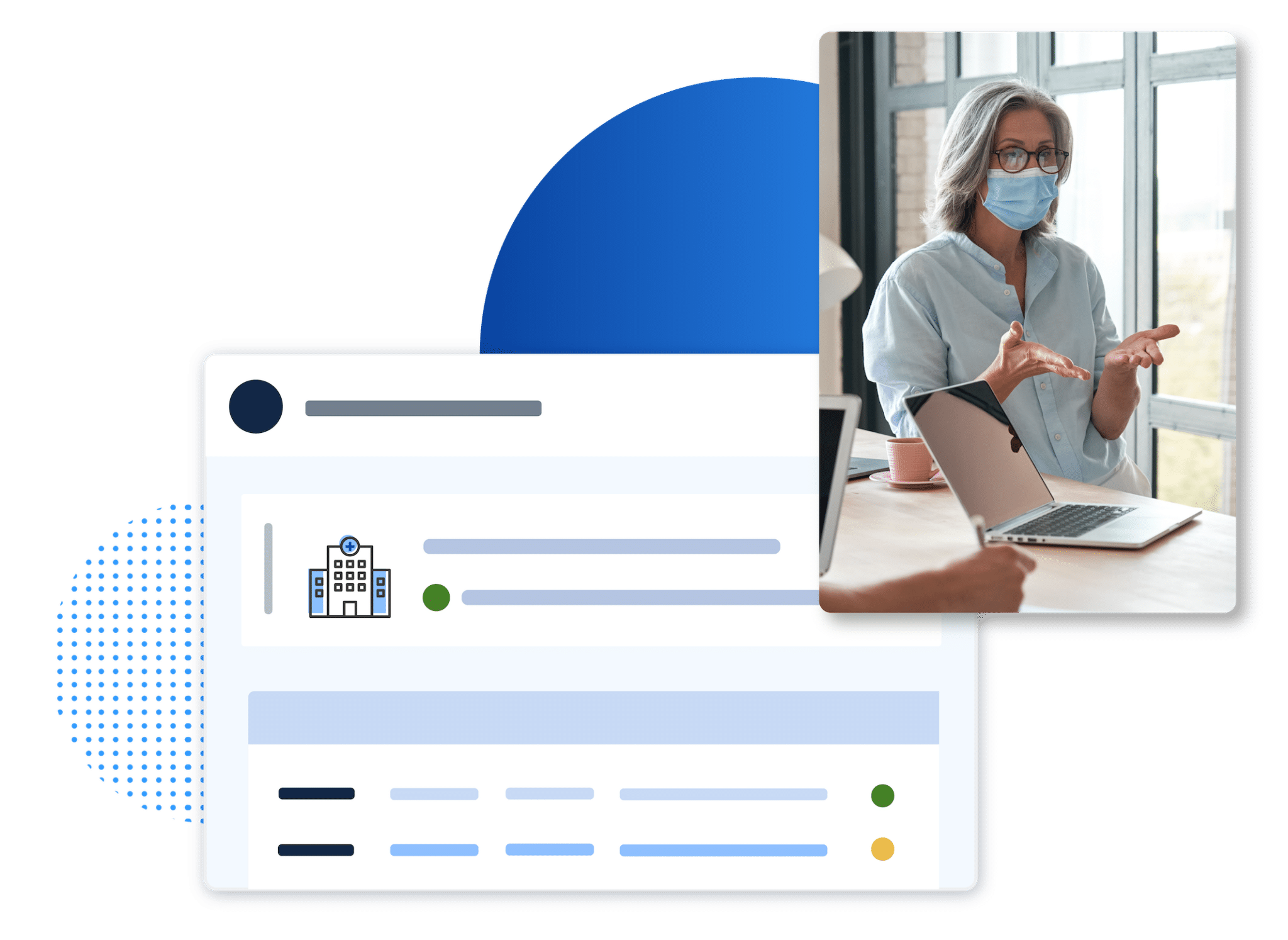
A Better Way to Credential Providers
0
%
of Primary Source Verifications Delivered within 2 Days
0
m+
Credential Verifications Performed Annually
0
m+
People & Entities Monitored Ongoing
Reliable Provider Credentialing at a Remarkable Pace
ProviderTrust’s HITRUST- and NCQA-certified provider credentialing solution ensures accurate, timely primary source verifications throughout the credentialing process.
Our data integrates directly into your existing workflows, removes the burden of manual verifications, and reduces credentialing turnaround times by 97%.
- Automated primary source verifications
- Results in less than 2 days
- API integrates into existing workflows
- Audit-ready documentation
- Improved provider experience
Reliable Results in a Fraction of the Time
Cut your initial turnaround time by 97%
Say goodbye to 60+ day turnaround times for initial credentialing. We return 95% of our primary source verifications in less than 2 days and the other 5% in less than a week.
Zero wait time for recredentialing results
After the initial check, all of your primary source verifications will be instant. Your credentialing team—and your provider network—will thank you.
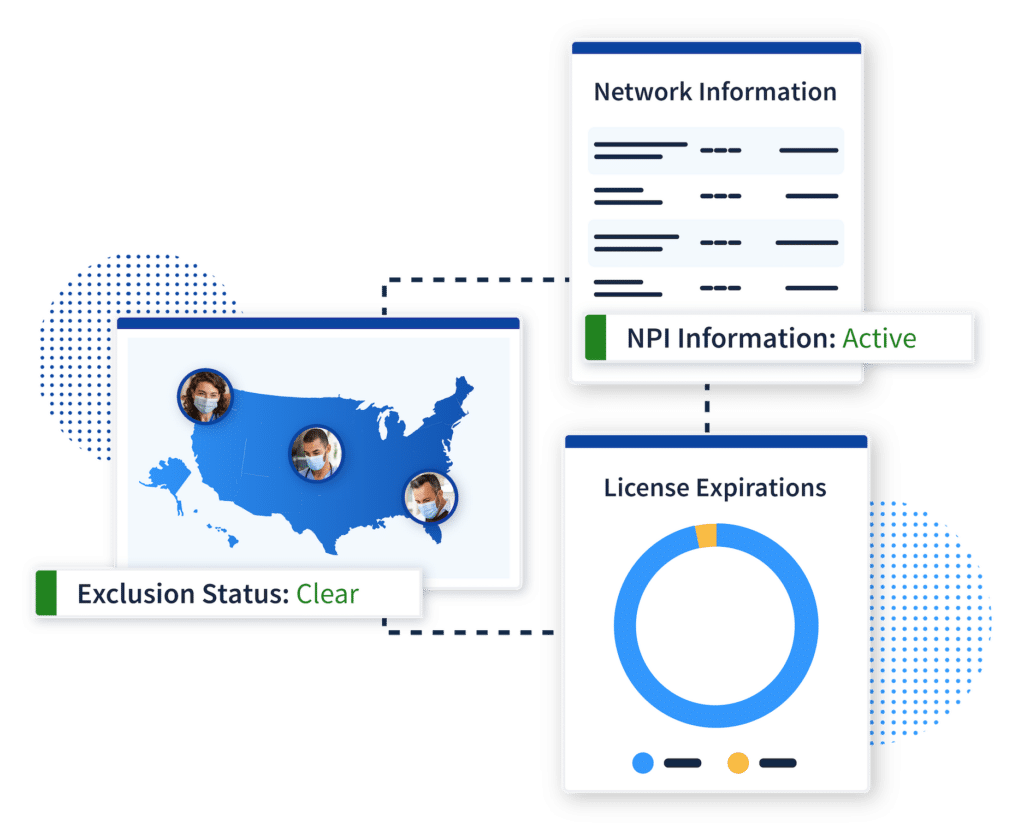

Our Data Makes a Difference
A data strategy that delivers accurate, complete results
Our proprietary data strategy enhances primary source data with unique identifiers to deliver an unbeatable level of accuracy. There are no “potential matches” to sort through because our data integrity ensures exact matches only.
A dynamic source of provider data
Don’t let your data go stale. Access verified credentials at any time with a secure API that fuels your existing workflows with ProviderTrust’s dynamic data, so you’ll always have the most up-to-date results.
Minimize Risk and Maximize Profit
Ongoing monitoring prevents unauthorized payments
We regularly monitor for exclusions between initial credentialing and recredentialing, so you don’t risk making payments to providers whose eligibility has changed since the last time you checked. Plus, we stand by our results with an E&O policy to give you peace of mind.
The highest standard of safety and security
We handle sensitive data every day, and we work hard to keep it secure. Our solutions are HITRUST- and NCQA-certified to ensure that our security practices meet and exceed the highest industry standards.




“Not only has ProviderTrust saved us countless hours of unnecessary work and delivered peace of mind, but their solution is also the most polished one that we work with. We’re frequently complimented on how organized our credentialing files and programs are.”
Data Integrity Built to Scale
Explore our monitoring and verification solutions, especially designed for Credentialing teams.

Provider Network Compliance
Eliminate compliance risk across your organization with a solution fueled by data that’s even better than the primary source.
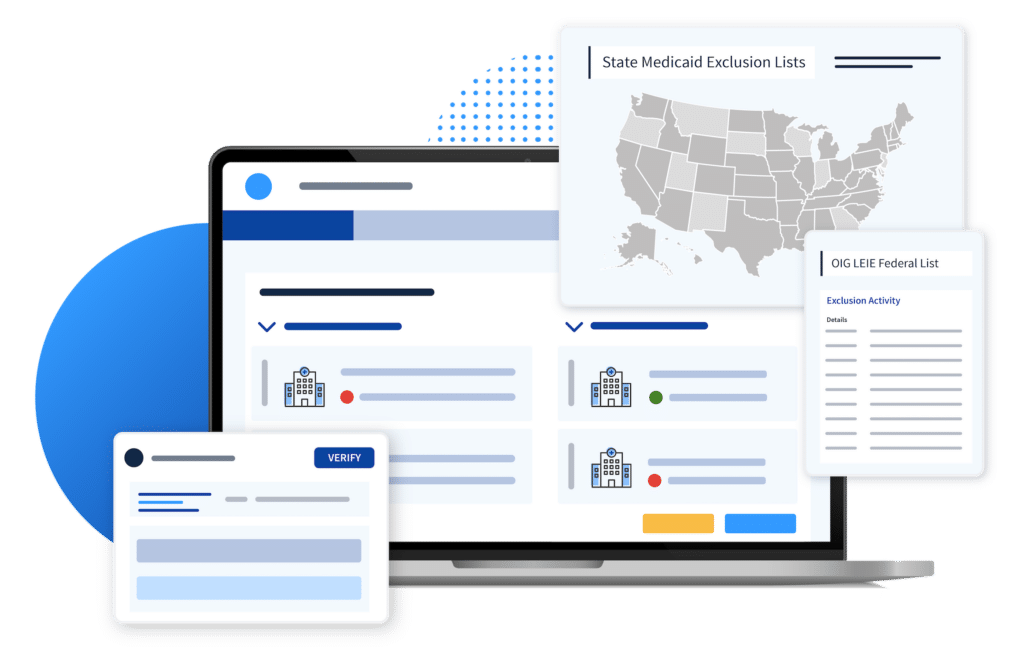
CVO Primary Source Verification
We monitor and verify compliance issues directly at the primary source across the healthcare ecosystem.
Related Resources
Webinars
The Changing Landscape of Credential Verification
Licenses and Credentials
Medicare and Medicaid
Payers
November 08, 2023
Read More
Case Studies
Trends, Challenges, and Opportunities Across Provider Credentialing
Licenses and Credentials
Payers
Providers
October 10, 2023
Read More
Blog
Provider Credentialing: What Payers Need to Know
Licenses and Credentials
Payers
April 14, 2023
Read More








